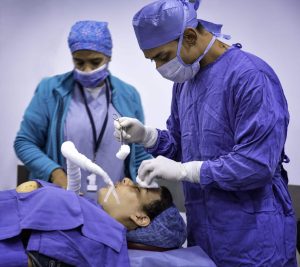
Several key advances have improved paramedic and EMT life-saving procedures in recent years, particularly in hemorrhage control, cardiac arrest resuscitation, trauma management, airway interventions, and technology integration. These build on evidence-based updates from organizations like the American Heart Association (AHA), International Liaison Committee on Resuscitation (ILCOR), and trauma guidelines, emphasizing faster, more targeted interventions in the prehospital setting.
1. Hemorrhage Control and Trauma Resuscitation
- Aggressive early hemorrhage control has shifted priorities: Techniques like tourniquets, wound packing, and the “X-ABC” or CAB (Circulation first, then Airway, Breathing) approach prioritize stopping massive bleeding before traditional ABC sequencing. Permissive hypotension (avoiding over-resuscitation with fluids) reduces coagulopathy risks.
- Tranexamic acid (TXA) administration in the field for traumatic hemorrhage has become more widespread, helping prevent or treat trauma-induced coagulopathy.
- Prehospital blood product resuscitation, including whole blood or balanced components, replaces heavy reliance on crystalloids. This “damage control resuscitation” approach improves survival in hemorrhagic shock from penetrating trauma or other causes.
- Intraosseous (IO) vascular access has advanced as a rapid, reliable alternative to IV lines, especially in shock or cardiac arrest when peripheral access fails.
- Resuscitative Endovascular Balloon Occlusion of the Aorta (REBOA): Select advanced prehospital teams (often HEMS or specialized units) now deploy this to temporarily control non-compressible torso hemorrhage (e.g., pelvic bleeding), raising blood pressure and buying time to definitive care. It has shown feasibility and potential to reduce prehospital cardiac arrest in exsanguinating patients.
- Finger thoracostomy (over traditional needle decompression) for tension pneumothorax offers better decompression in trauma.
Emerging concepts like Selective Prehospital Advanced Resuscitative Care (SPARC) teams aim to bring physician- or paramedic-led advanced interventions (blood, REBOA, advanced airway) closer to the point of injury.
2. Cardiac Arrest Management
- 2025 AHA Guidelines updates emphasize high-quality CPR with refinements in compression-to-ventilation ratios, early defibrillation, and considerations for advanced airways. There is renewed focus on avoiding hyperventilation and optimizing team dynamics. Some updates include starting compressions while assessing reversible causes in certain device-related arrests.
- Mechanical CPR devices (e.g., LUCAS or AutoPulse) provide consistent, high-quality chest compressions during prolonged resuscitation or transport, freeing providers for other tasks.
- Point-of-Care Ultrasound (POCUS) in the field helps identify reversible causes (e.g., pericardial effusion, pneumothorax) or guide procedures.
- Drone-delivered AEDs: Programs in various regions (e.g., trials in the US, Sweden, and others) launch drones carrying automated external defibrillators to cardiac arrest scenes faster than ground EMS, potentially shortening time to first shock in rural or congested areas.
3. Airway and Sedation Advances
- Ketamine has gained prominence for prehospital sedation, analgesia, and rapid sequence intubation (RSI) due to its hemodynamic stability compared to some alternatives. Studies compare it favorably to midazolam for agitation or procedural sedation, with similar safety profiles regarding airway interventions, though ketamine may provide deeper sedation.
- Refined protocols for advanced airway management (supraglottic airways or endotracheal intubation) balance the need for oxygenation with minimizing interruptions in CPR. Some data suggest benefits from higher levels of EMS providers performing these skills.
4. Technology and Systems Innovations
- Portable ultrasound and capnography (continuous ETCO2 monitoring) improve diagnostic accuracy and confirm airway placement or CPR quality in the field.
- Telemedicine and real-time data transmission allow paramedics to consult with physicians or specialists en route, supporting complex decisions.
- AI-assisted decision support and enhanced dispatch systems optimize response and resource allocation.
- Non-transport ALS or “paramedic intercept” programs: Advanced providers respond quickly (sometimes via fire apparatus or motorcycles) to deliver interventions before standard ambulances arrive, improving outcomes in time-sensitive cases like cardiac arrest or sepsis (e.g., early antibiotics in some systems).
- Drone delivery extends beyond AEDs to experimental blood product transport in remote or austere environments.
Broader Impacts
Higher-trained crews (paramedics vs. basic EMTs) correlate with better neurologic outcomes in out-of-hospital cardiac arrest in some large studies. Expanded scopes in certain regions allow paramedics greater autonomy with medications, procedures, and protocols tailored to local needs.
These advances focus on minimizing preventable deaths from exsanguination, improving perfusion during resuscitation, and leveraging technology for faster, smarter care. Implementation varies by region, training level, and system resources—EMTs generally focus on basic life support (BLS) with some expansions, while paramedics handle advanced life support (ALS) procedures like IV/IO meds, advanced airways, and monitoring.